As a certified lymphedema therapist (CLT-LANA), a big part of my work is helping people understand how to prevent lymphedema and lower their chances of developing this chronic condition.
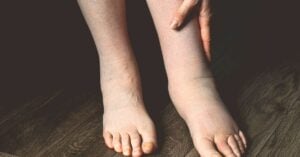
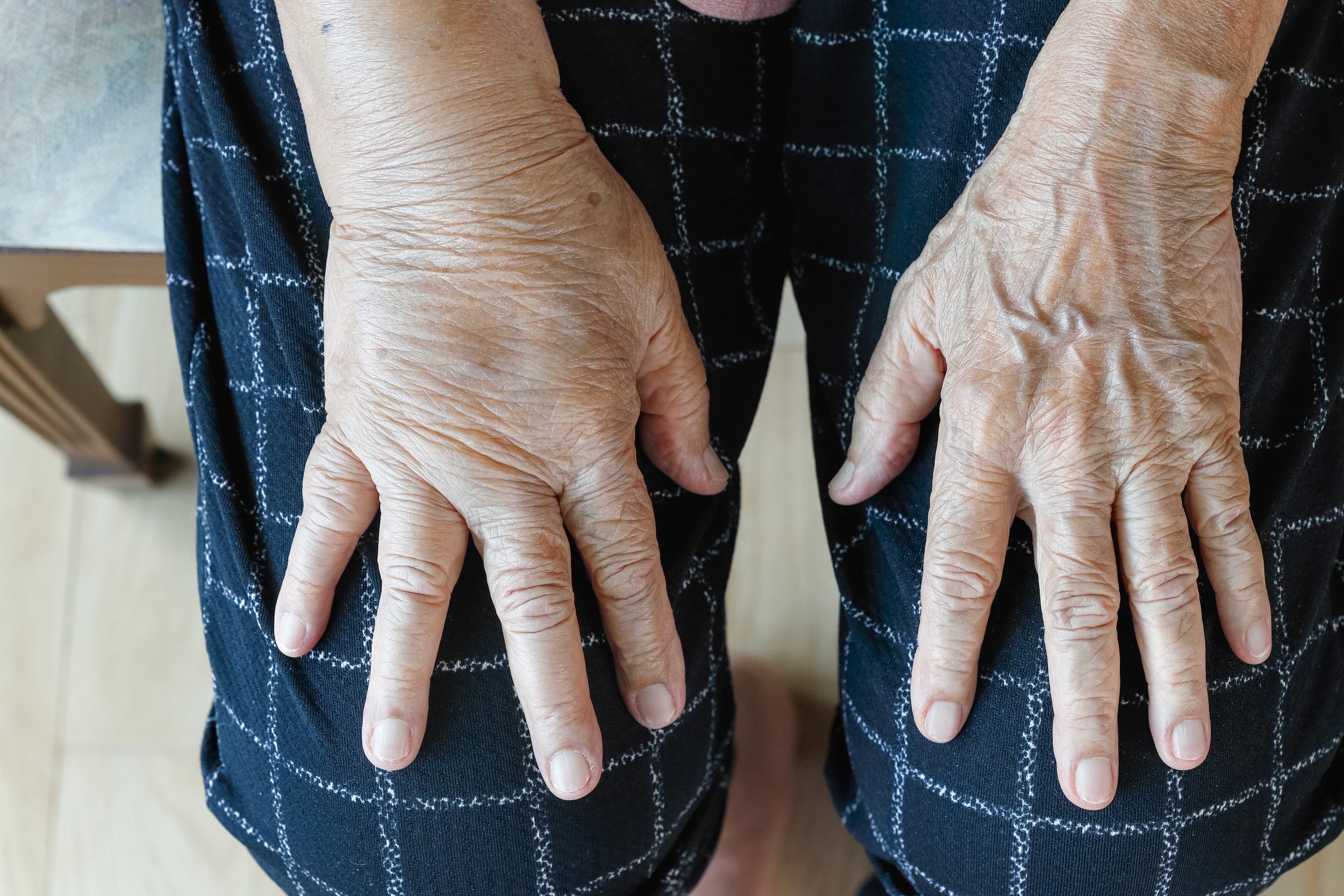
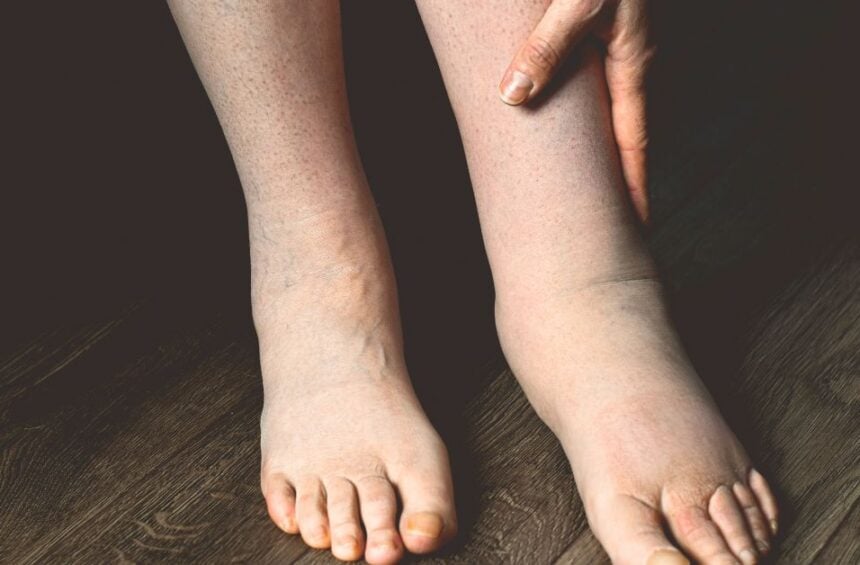
Lymphedema causes swelling in your arms, legs, or other parts of your body.
If you’ve had lymph nodes removed or received radiation therapy, you have a higher risk of developing this condition, but that doesn’t mean it’s inevitable. There are practical steps you can take to support your lymphatic system.
Let’s take a closer look at them.
What Is Lymphedema?
Lymphedema is a chronic condition in which lymphatic fluid builds up in your tissues and causes swelling. Your lymphatic system normally drains this fluid. But when it gets damaged or blocked, a lot of excess fluid can accumulate, which feels uncomfortable and sometimes painful.
Lymphedema most commonly affects your arm or leg, but it can develop in other areas like your chest, neck, abdomen, or genitals, depending on where your lymph nodes were affected.
Common lymphedema symptoms include:
- Swelling in your arm, leg, or other affected area
- A feeling of heaviness or tightness
- Reduced range of motion
- Skin that feels tight or looks shiny
- Aching or pain in the swollen area
- Thickened or hardened skin over time
There are two main types of lymphedema, primary and secondary.
Primary lymphedema is a rare genetic condition where your lymphatic system doesn’t develop properly. It can show up at any age, from infancy to adulthood, but it only affects 1 in 100,000 people.
Secondary lymphedema develops when something damages your lymphatic system, like surgery, radiation, or infection. It’s much more common, affecting approximately 1 in 1,000 Americans.
Learn more about the different stages of lymphedema.
Risk Factors for Developing Lymphedema
Many factors increase your chances of developing lymphedema, including:
- Surgery: Procedures that remove or damage lymph nodes, like sentinel lymph node biopsy or cancer-related surgeries, can disrupt how lymph fluid drains from your body.
- Breast cancer treatment: Breast cancer surgery and radiation are among the most common causes of lymphedema in the arms.
- Radiation therapy: Radiation can scar and inflame your lymph nodes and vessels, which blocks proper drainage and can lead to side effects like radiation fibrosis.
- Infections: Bacterial infections like cellulitis cause inflammation that damages your lymphatic system, so treating infections quickly is important.
- Obesity: Extra weight puts pressure on your lymphatic system and makes it harder for lymph fluid to drain properly.
- Inactivity: Sitting or lying down for long periods slows lymph flow, which is one of the reasons why people often experience swelling after surgery.
- Genetics: A family history of lymphedema means your lymphatic system may not function as well, making you more vulnerable when other risk factors are present.
Even if you have multiple risk factors, you can take steps to reduce your chances of developing lymphedema. Not everyone at risk develops lymphedema—many people who have lymph nodes removed or receive radiation never experience it.
👉 Follow this Breast Cancer Recovery Roadmap to prevent lymphedema after breast cancer treatment.
Looking for more lymphedema tips? Join my newsletter!
How to Prevent Lymphedema: Tips from a Certified Lymphedema Therapist (CLT-LANA)
The best way to prevent lymphedema is to support your lymphatic system and help it drain properly. You don’t need to detox or do anything intense, but simple habits like regular movement can make a big difference.
Here are the best lymphedema prevention strategies I recommend as a certified lymphedema therapist (CLT-LANA).
1. Maintain a Healthy Weight
Carrying extra weight puts strain on your lymphatic system and makes it harder for fluid to drain. This is why maintaining a healthy weight is one of the most effective ways to reduce your lymphedema risk.
Focus on eating a balanced, healthy diet with plenty of fruits, vegetables, lean proteins, and whole grains. Limit salt, sugar, and unhealthy fats. When you exercise regularly and eat well, you support both your lymphatic function and your immune system.
Learn more about a lymphedema-friendly diet.
2. Stay Active
Physical activity improves lymphatic drainage and keeps fluid moving through your body. Low-impact exercises like walking, swimming, or cycling work well for people at risk of lymphedema.
If you’re recovering from cancer treatment or breast surgery, start with just a few minutes of movement each day. Gradually work up to 25-30 minutes of physical activity. It’s important to set realistic goals instead of pushing yourself too hard, too fast.
I have helpful exercise guides for different areas of the body that can help you stay active safely:
Learn more about the best exercise for lymphatic drainage.
3. Try Vibration Plates
Vibration plates are platforms that vibrate at different frequencies when you stand, sit, or place your hands or feet on them. These vibrations create gentle muscle contractions that help move lymph fluid through your body.
For lymphatic drainage, use low-frequency settings (around 10-12 hertz) for 5-10 minutes at a time. The gentle vibrations stimulate your lymphatic vessels without being too intense. Many people find that regular vibration plate use helps reduce swelling and improve circulation.
You can also start with these vibration plate exercises for beginners.
4. Try Rebounders
A rebounder is a small trampoline you can use for bouncing. The up-and-down movement creates changes in gravitational pull that help pump lymph fluid through your body.
Even gentle bouncing or simply shifting your weight from foot to foot on the rebounder stimulates lymph flow. It’s low-impact, easy on your joints, and can be done in your living room while watching TV.
5. Dry Brush
Dry brushing involves using a soft-bristled brush on your dry skin in gentle strokes. This technique stimulates your lymphatic system and encourages drainage.
Always brush toward your lymph nodes. For example, brush from your hands up toward your armpits, or from your feet up toward your groin. Use light pressure and brush in long, smooth strokes. The key is to be gentle—you’re not scrubbing, just lightly stimulating the skin and the lymphatic vessels underneath.

Dry Brushing to the Neck and Face for a Healthy Lymphatic System – Digital
6. Do Lymphatic Drainage Massage
Lymphatic drainage massage uses light, rhythmic strokes to move lymph fluid toward your lymph nodes.
You can learn simple self-massage techniques to use at home, or work with a certified lymphedema therapist who can teach you the proper movements. The pressure should be very light—much lighter than a regular massage.
See this before and after a lymphatic drainage massage.
7. Practice Good Skin Care
Skin infections can trigger lymphedema, especially when you’re recovering from cancer treatment or surgery. Make sure to keep your skin clean and protected:
- Keep your skin moisturized daily to prevent dryness and cracking.
- Wear gloves when doing dishes, gardening, or cleaning to protect your hands from cuts and irritation.
- Clean any cuts or scrapes immediately and apply antiseptic cream, even if they’re small.
- Use an electric razor instead of a blade to avoid nicks and cuts.
- File your nails instead of cutting them, and avoid sharp tools during manicures or pedicures.
- Avoid using harsh soaps or chemicals that can irritate your skin.
These tips may seem basic, but when your lymphatic system is compromised, even minor infections can become bigger problems.
8. Don’t Wear Tight Clothing
Tight clothing and accessories can restrict lymphatic flow and increase swelling. Wear loose-fitting, comfortable clothes that allow proper circulation and lymphatic drainage. Avoid wearing jewelry like tight bracelets or rings that dig into your skin.
This might sound confusing if you’ve heard about compression garments for lymphedema. The difference is that medical compression garments are designed to support lymphatic drainage. Regular tight clothing and accessories don’t provide that same benefit. They just restrict flow.
If your doctor recommends compression garments, those are safe to wear. Just avoid everyday tight clothing and accessories on areas at risk for lymphedema.
9. Avoid Insect Bites
Bug bites can lead to infections and inflammation, which increases your lymphedema risk.
Use insect repellent when you’re outside, especially during peak bug hours, and wear long sleeves and pants in areas where insects are active. If you do get a bite, treat it quickly with antiseptic cream to prevent infection
10. Don’t Get Too Hot or Too Cold
Extreme temperatures can affect how well your lymphatic system works. If you’re at high risk of developing lymphedema, do your best to keep your body temperature stable.
Avoid hot tubs, hot baths, saunas, and steam rooms because heat causes blood vessels to dilate, which can lead to more swelling. It’s also important to avoid sunburn.
On the flip side, don’t expose yourself to extremely cold temperatures for long periods and dress appropriately for the weather.
How to Prevent Lymphedema After Mastectomy
Mastectomy increases your lymphedema risk because removing lymph nodes disrupts normal drainage, but you can take steps to lower your chances of developing the condition:
- Start gentle exercises as soon as your doctor clears you to help keep lymph fluid moving through your body.
- Wear compression garments like sleeves if your healthcare provider recommends them to support drainage and prevent fluid buildup.
- Practice good skin care and treat any cuts or infections immediately to avoid complications.
- Avoid heavy lifting or strenuous activities with your affected arm until you’ve built up strength gradually.
- Keep your arm elevated when resting to help reduce swelling and promote drainage.
If you don’t know where to start with exercise after a mastectomy, I created these helpful guides:
👉 For more in-depth support, learn more about Breast Cancer Rehab!
How to Prevent Lymphedema After Lymph Node Removal
Lymph node removal disrupts normal lymphatic flow, which can trigger lymphedema. Take these steps to minimize your risk:
- Start gentle exercises as soon as your doctor gives you the go-ahead
- Avoid having blood pressure readings taken, blood draws, or injections on the affected limb
- Practice good skin care and treat cuts and scrapes right away
Lymph node removal is common during breast cancer treatment. While breast cancer is often thought of as a women’s health issue, men can get breast cancer and develop lymphedema as well.
Learn more about lymphedema in men after breast cancer treatment.
What Are the First Signs of Lymphedema?
Catching lymphedema early makes treatment a lot more effective. Watch for these early warning signs:
- Mild swelling that comes and goes
- A feeling of heaviness or fullness in your arm, leg, or other affected area
- Tightness in your skin or the sensation that your skin feels different
- Reduced flexibility or range of motion in nearby joints
- Clothing, shoes, or jewelry that suddenly feels tighter than usual
- Aching or discomfort in the affected area
If you notice any of these signs, contact your healthcare provider as soon as possible. Early intervention makes it much easier to manage lymphedema symptoms. Sometimes, it can even naturally reverse swelling.
Lymphedema Treatment
If you do develop lymphedema, there’s no cure, but management is very effective.
Complete decongestive therapy (CDT) is the gold standard treatment for lymphedema. This approach includes a few different things:
- Manual lymphatic drainage
- Compression therapy
- Physical exercise
- Skin care
During the first phase of treatment, you’ll work with a certified lymphedema therapist. This intensive phase typically lasts several weeks and focuses on reducing your swelling as much as possible.
After the initial treatment phase, you’ll continue with lymphedema self-care at home using compression garments, exercise, skin care, and self-massage techniques.
Learn more about lymphedema treatment.
Looking for More Support?
Working with a certified lymphedema therapist can make a big difference if you’re at risk for or already experiencing lymphedema. They can create a plan with exercises, compression therapy, and manual lymphatic drainage to reduce your swelling and symptoms.
But unfortunately, many people don’t have access to a certified lymphedema therapist or proper care.
That’s why I created online, self-paced programs like Lower Body Lymphedema Rehab and Breast Cancer Rehab.
These programs give you the same tools and exercises I use with my physical therapy clients, adapted so you can do them at home and take control of your lymphedema prevention and management.
Learn more about Lower Body Lymphedema Rehab and Breast Cancer Rehab!